[HOME PAGE] [STORES] [CLASSICISTRANIERI.COM] [FOTO] [YOUTUBE CHANNEL]
 |  |  |
| | ||
Medical Encyclopedia |
|
| Other encyclopedia topics: | A-Ag Ah-Ap Aq-Az B-Bk Bl-Bz C-Cg Ch-Co Cp-Cz D-Di Dj-Dz E-Ep Eq-Ez F G H-Hf Hg-Hz I-In Io-Iz J K L-Ln Lo-Lz M-Mf Mg-Mz N O P-Pl Pm-Pz Q R S-Sh Si-Sp Sq-Sz T-Tn To-Tz U V W X Y Z 0-9 |
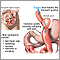
Gastric bypass surgery
| Contents of this page: | |
Illustrations
|
|
|
|
|
|
Alternative Names Return to top
Bariatric surgery - gastric bypass; Roux-en-Y gastric bypass; Gastric bypass - Roux-en-YDefinition Return to top
Gastric bypass is surgery that is done to help you lose weight. After the surgery, you will not be able to eat as much as before, and your body will not absorb all the calories from the food you eat.
See also: Laparoscopic gastric banding
Description Return to top
This surgery helps you lose weight by changing how your stomach and small intestine handle the food you eat.
- After the surgery, your stomach will be smaller. You will feel full or satisfied with less food.
- The food you eat will no longer go into some parts of your stomach and small intestine that break down food. Because of this, your body will not absorb all the calories from the food you eat.
You will receive general anesthesia before this surgery. This will make you unconscious and unable to feel pain.
Gastric bypass can be done in 2 ways. In open surgery, your surgeon will make a large incision (cut) to open up your belly. Your surgeon will do the bypass by directly handling your stomach, small intestine, and other organs.
Another way to this surgery is to use a tiny camera, called a laparoscope, which is placed in your belly. This is called laparoscopy. In this surgery:
- First, your surgeon will make 4 to 6 small incisions in your belly.
- Then your surgeon will pass the laparoscope through one of these incisions. It will be connected to a video monitor in the operating room. Your surgeon will look at the monitor to see inside your belly.
- Your surgeon will use thin surgical instruments to do your bypass. These instruments will be inserted through the other incisions.
- You will probably stay in the hospital a shorter time and recover more quickly after laparoscopy, compared to open surgery. There are also fewer incision problems after this surgery. You will also have smaller scars and a lower risk of developing hernias after laparoscopic surgery.
Laparoscopy may not be safe for you if you:
- Have had abdominal surgery in the past. This is because you may have scar tissue from earlier surgery.
- Have severe heart and lung disease
- Weigh more than 350 pounds
There are 2 basic steps during both kinds of gastric bypass:
- The first step makes your stomach smaller. Your surgeon will use staples to divide your stomach into a small upper section and a larger bottom section. The top section of the stomach (called the pouch) is where the food you eat will go. This pouch is about the size of a walnut. It holds only about 1 ounce of food.
- The second step is the bypass. Your surgeon will connect a part of your small intestine, called the jejunum, to a small hole in your pouch. The jejunum is farther down from where your stomach normally attaches to your small intestine. Food you eat will now travel from the pouch into this new opening into your small intestine. When food travels this way, it bypasses the lower part of your stomach and the first part of your small intestine. Because of this, your body will absorb fewer calories.
This surgery takes about 4 hours.
This surgery may increase your risk for gallstones. Your doctor may recommend having a cholecystectomy (surgery to remove your gallbladder) before your bypass surgery.
Why the Procedure is Performed Return to top
Weight-loss surgery may be an option if you are very obese and have not been able to lose weight through diet and exercise.
Gastric bypass surgery is not a "quick fix" for obesity. You must be committed to diet and exercise because you must continue dieting and exercising after the surgery. You may have complications from the surgery if you don’t. One problem some people have is throwing up if they eat more than their new small stomach can hold.
People who have this surgery should be mentally stable and not be dependent on alcohol or illegal drugs.
This procedure may be recommended for you if you have:
- A body mass index (BMI) of 40 or more. Someone with a BMI of 40 or more is at least 100 pounds over their recommended weight. A normal BMI is between 18.5 and 25.
- A BMI of 35 or more and a serious medical condition that might improve with weight loss. Some of these conditions are sleep apnea, type 2 diabetes, and heart disease.
Risks Return to top
Gastric bypass is major surgery and has many risks. Some of these risks are very serious. You should discuss these with your surgeon.
The risk of the surgery itself or for problems after surgery may be greater than normal if you are:
- Unable to walk even short distances. This increases your risk of blood clots, lung problems, and pressure sores (also called bed sores).
- A child who is still growing
- An adult older than 60 to 65 years
Risks for any anesthesia are:
- Allergic reactions to medicines
- Breathing problems
Risks for any surgery are:
- Blood clots in the legs that may travel to your lungs
- Infection, including in the incision, lungs (pneumonia), bladder, or kidney
- Blood loss
- Heart attack or stroke during surgery
Risks or problems that may occur during or soon after gastric bypass surgery are:
- Injury to the stomach, intestines, or other organs during surgery
- Leaking through the staples in the stomach after surgery. This may require an emergency surgery.
- Depression
The risks or problems of weight-loss surgery that may occur over time are:
- Breakdown of the pouch, which would require another surgery to repair it
- The opening between your stomach pouch and the small intestine may get narrower. This could require another surgery.
- Anemia from low iron or vitamin B12 levels
- Low calcium levels, which can cause early osteoporosis or other bone disorders
- Gallstones and gallbladder attacks, which occur more often when you lose weight quickly.
- Gastritis (inflamed stomach lining), heartburn, or stomach ulcers
- Poor nutrition
- Vomiting from eating more than your stomach pouch can hold
- Dumping syndrome. This is when the contents in your stomach move through your small intestine quickly. This causes discomfort and poor nutrition.
- Incisional hernia, which is much more common when an open procedure is done. An incisional hernia is a bulging of tissue through the site of your incision.
- Kidney stones
Before the Procedure Return to top
Your surgeon will ask you to have tests and visits with your other health care providers before you have this surgery. Some of these are:
- A complete physical exam
- Blood tests, ultrasound of your gallbladder, and other tests to make sure you are healthy enough to have surgery
- Visits with your doctor to make sure other medical problems you may have, such as diabetes, high blood pressure, and heart or lung problems, are under control
- Nutritional counseling
- Classes to help you learn what happens during the surgery, what you should expect afterward, and what risks or problems may occur afterward
- Visiting with a mental health provider to make sure you are emotionally ready for major surgery. You must be able to make major changes in your lifestyle after surgery.
If you are a smoker, you should stop smoking several weeks before surgery and not start smoking again after surgery. Smoking slows recovery and increases the risks of problems. Tell your doctor or nurse if you need help quitting.
Always tell your doctor or nurse:
- If you are or might be pregnant
- What drugs, vitamins, herbs, and other supplements you are taking, even ones you bought without a prescription
During the week before your surgery:
- You may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), vitamin E, warfarin (Coumadin), and any other drugs that make it hard for your blood to clot.
- Ask your doctor which drugs you should still take on the day of your surgery.
- Prepare your home for after the surgery
On the day of your surgery:
- Do not eat or drink anything after midnight the night before your surgery.
- Take the drugs your doctor told you to take with a small sip of water.
- Your doctor or nurse will tell you when to arrive at the hospital.
After the Procedure Return to top
Most people stay in the hospital for 3 to 5 days after surgery. In the hospital you:
- Will be asked to sit on the side of the bed and walk a little the same day you had surgery
- May have a catheter (tube) that goes through your nose into your stomach for 1 or 2 days. This tube helps drain fluids from your belly.
- Will not be able to eat for the first 1 to 3 days. After that you can have liquids, and then puréed or soft foods after that.
- May have a catheter connected to the larger part of your stomach that was bypassed. It will come out of your side and will drain fluids.
- Will wear special stockings on your legs to help prevent blood clots from forming.
- Will receive medicine through shots to prevent blood clots
- Will receive pain medicine. You will take pills for pain or receive pain medicine through an IV, a catheter that goes directly into your veins.
You will be able to go home when you:
- Can eat liquid or puréed food without vomiting
- Can move around without a lot of pain
- Do not need pain medicine through an IV or given by shot
Outlook (Prognosis) Return to top
Most people lose about 10 to 20 pounds a month in the first year after surgery. Weight loss will decrease over time, so sticking to your diet and exercise early on will provide the largest weight loss. You may lose half or more of your extra weight in the first 2 years. You will lose weight most quickly just after surgery, when you are still on a liquid diet or pureed diet.
Losing enough weight after surgery can improve many medical conditions you might also have. Conditions that may improve are asthma, type 2 diabetes, high blood pressure, obstructive sleep apnea, high cholesterol, and gastroesophageal disease (GERD).
Weighing less should also make it much easier for you to move around and do your everyday activities.
Bypass surgery alone is not a solution for weight loss. It can train you to eat less, but you still have to do much of the work. To lose weight and avoid complications from the procedure, you will need to follow the exercise and eating guidelines that your doctor and dietitian gave you.
References Return to top
Buchwald H, Estok R, Fahrbach K, Banel D, Sledge I. Trends in mortality in bariatric surgery: a systematic review and meta-analysis. Surgery, 2007;142:621-632.
Leslie D, Kellogg TA, Ikramuddin S. Bariatric surgery primer for the internist: keys to the surgical consultation. Med Clin North Am. 2007;91:353-381.
Townsend Jr. CM, Beauchamp RD, Evers BM, Mattox KL. Townsend: Sabiston Textbook of Surgery. 18th ed. Philadelphia, Pa: Saunders; 2008.
Update Date: 2/12/2009 Updated by: Crystine Lee, MD, Department of Surgery, Marin General Hospital, Greenbrae, CA. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.

The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2009, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
EDIZIONI DI PUBBLICO DOMINIO (HTML)
- Alighieri - La Divina Commedia
RISORSE DAL WEB:
Encyclopaedia Britannica 1911 - PDF
Project Gutenberg: DVD-ROM 2007
Wikipedia for Schools - ENGLISH
Wikipedia for Schools - FRENCH
Wikipedia for Schools - SPANISH